UOG assists UCSF in training 94 contact tracers
UOG assists UCSF in training 94 contact tracers
UOG assists UCSF in training 94 contact tracers
9/24/2020

A total of 94 government employees, health care workers, private school employees, University of Guam students, and volunteers are now assisting the island’s contact tracing efforts following the completion of a four-day training with the chief medical officer for the University of California San Francisco.
The trainees are now able to supplement the work of the island’s 20 investigators and 24 contact tracers.
“With these additional contact tracers, people can anticipate receiving their results more quickly, getting contacted sooner if they were potentially exposed to a known COVID-19 case, and, ultimately, greater peace of mind for themselves and their loved ones,” said Arthur U. San Agustin, acting director of the Department of Public Health and Social Services.

The training, which was held virtually from Aug. 3–7, was the first of an ongoing partnership between UCSF and the Office of the Governor, DPHSS, and the University of Guam.
“Contact tracing is essential for containing any communicable disease outbreak. This is especially useful for COVID-19, which can be spread by people who have no symptoms,” Gov. Lou Leon Guerrero said. “But contact tracing can be a long and vigorous process, and our contact tracing team has been working nonstop since the beginning of this pandemic to keep us safe. By partnering with the University of Guam, we are now able to supplement our current resources, increase our capacity, and move forward in our response and recovery.”
The participants were taught by Dr. Michael J. Reid and Laura Buback, who holds a master’s in public health, who through the UCSF’s Pandemic Initiative for Equity and Action work with local governments to produce more integrated, sustainable, and responsive health systems.
“We have to close in on this pandemic from multiple angles, and building our human
capacity to effectively track cases through the training of the experienced professionals
from UCSF is a big part of the solution,” said Margaret Hattori-Uchima, dean of the
School of Health at UOG, which coordinated, provided support for, and recruited participants for the
training. “UOG is grateful to have helped facilitate this training and will continue
to be available to support the community effort against COVID-19 going forward.”


“If you could reach and instantaneously notify and isolate 60% of patients with symptoms before they infect anybody else and instantaneously trace over 50% of their contacts and isolate/quarantine them before they infect anybody, you control the epidemic,” Reid said, citing research by the University of Oxford (U.K.). “However, if you have a delay of two days in both isolation of infected individuals and quarantine of exposed individuals, then you need to trace at least 70% to 90% of contacts to stop the epidemic — it becomes far more challenging.”
For manual contact tracing, Buback said it is important to first establish the onset date of the infected person’s symptoms and/or test date in order to determine the infectious period. The infectious period begins two days before the onset of symptoms or two days before the person’s test date in asymptomatic cases.
The tracers can then ask about the places and people affected within that person’s infectious period. Ideally, Buback said, contacts of infected individuals should be contacted within 24 hours or within the same day of being reported to the health department to reduce the time for potentially infectious individuals to be in public.
Those contacted will be informed of their exposure to COVID-19 but not the personal information of who has tested positive. They will be referred for testing, connected to resources to facilitate a safe quarantine at home, and given information to monitor themselves for symptoms.
Contact tracing is “not a silver bullet,” Reid said, but it significantly reduces the spread when done in tandem with access to testing and isolation and quarantine resources, such as housing, food, and social services.
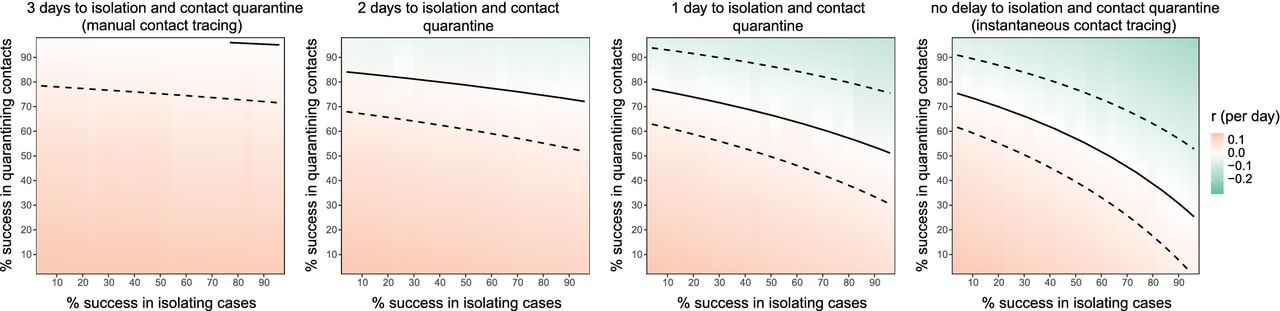
Heat maps show the impact of instantaneous contact tracing versus having a one- to three-day delay in isolating and quarantining infected and exposed individuals. Sourced from University of Oxford research published on May 8 in Science journal
The Hilton Guam Resort & Spa and United Airlines sponsored accommodations and travel for the University of California San Francisco team through the UOG Endowment Foundation.

